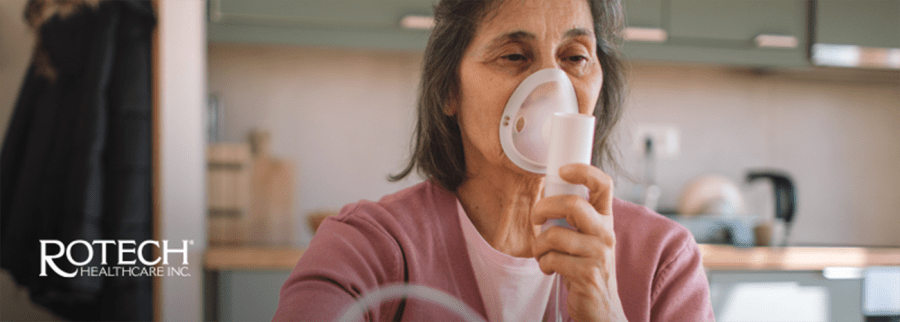You’re carrying laundry up the stairs. Halfway up, your chest tightens. Breathing feels shallow, effortful. You stop, grip the railing, wait for it to pass.
Or maybe it happens when you’re getting dressed in the morning, bending over to tie your shoes, or walking across a parking lot on a humid day.
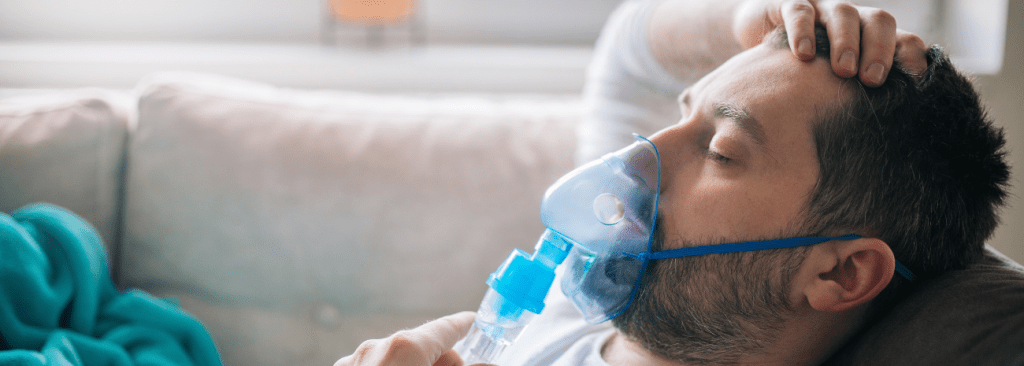
If you live with chronic obstructive pulmonary disease (COPD), moments like these are familiar, and unsettling. The sensation of not being able to get enough air can trigger worry, frustration, and sometimes panic, which only makes breathing harder.
This article focuses on practical, everyday strategies for managing shortness of breath at home. Not quick fixes, but approaches that can help you feel more in control when breathing becomes difficult, and habits that may support easier breathing over time.
What Shortness of Breath Feels Like in COPD
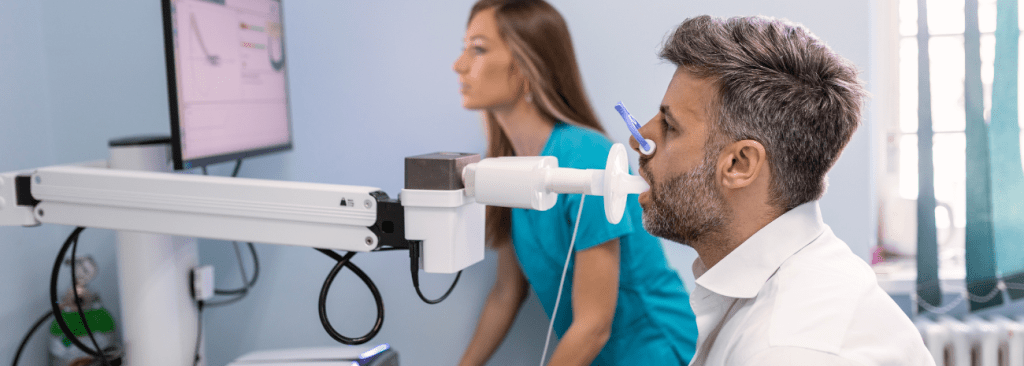
Chronic obstructive pulmonary disease (COPD) is a long‑term lung condition that makes it harder to move air in and out of the lungs. It includes conditions like emphysema and chronic bronchitis, and it often causes ongoing shortness of breath that can worsen with activity or illness.
COPD affects the airways and air sacs in your lungs, making it harder for air to move in and out. Over time, this can cause breathlessness during activities that once felt routine.
People describe the sensation differently. Some feel tightness in the chest. Others experience what’s sometimes called “air hunger” — a feeling of not being able to take a satisfying breath. Fatigue often accompanies it, because breathing requires more effort than it should.
Symptoms can vary day to day, even hour to hour. Weather, activity level, sleep quality, stress, and exposure to irritants all play a role. A good morning doesn’t mean the afternoon will be easy, and a difficult day doesn’t necessarily signal that something has changed with your condition.
Understanding this variability can help reduce some of the anxiety that comes with unpredictable symptoms. Fluctuation is part of living with COPD, not necessarily a sign that things are getting worse.

What to Do in the Moment When Breathing Feels Difficult
When shortness of breath hits, having a few reliable strategies can help you regain a sense of control.
Pursed-Lip Breathing
This technique slows your breathing and helps keep airways open longer, making each breath more effective.
How to do it:
- Breathe in slowly through your nose for about 2 seconds
- Purse your lips as if you’re about to blow out a candle
- Breathe out slowly and gently through your pursed lips for 4–6 seconds
- Repeat until your breathing feels more controlled
Pursed-lip breathing works best when you practice it regularly, not just during episodes. The more familiar it becomes, the easier it is to use when you really need it.
Positioning Your Body
Certain positions can ease the work of breathing by giving your diaphragm more room to move.
- Standing: Lean forward slightly with your hands resting on a table, counter, or your thighs
- Sitting: Lean forward with your elbows on your knees or on a table in front of you
- Resting: Lie on your side with pillows supporting your head and between your knees
Find what works for you. Different positions help different people, and what helps may vary depending on the situation.
Slow Down and Pause
When you feel breathless, the instinct is often to push through. But continuing activity can make symptoms worse.
Stop what you’re doing. Sit or lean if you can. Give your breathing time to settle before deciding whether to continue, modify, or rest.
Everyday Habits That Support Easier Breathing
Beyond in-the-moment strategies, certain daily habits can help reduce how often breathlessness disrupts your day.
Plan Activities to Conserve Energy
Pacing yourself matters. Break tasks into smaller steps with rest periods in between. Tackle more demanding activities earlier in the day when energy is often higher. Sit down for tasks when standing isn’t necessary.
This kind of planning is all about doing things in a way that works with your breathing, not against it.
Stay Consistent With Prescribed Therapy
If you use inhalers, nebulizers, or supplemental oxygen, using them as prescribed helps keep symptoms more stable. Skipping doses or using equipment inconsistently can make breathlessness harder to manage.
If you’re unsure whether your current therapy is working, or if you’re having trouble using your equipment correctly, talk with your care team. Small adjustments can sometimes make a meaningful difference.
Create a Comfortable Home Environment
Indoor air quality matters more than most people realize. Reducing dust, avoiding strong fragrances, and keeping humidity at a comfortable level can all help.
If outdoor air quality is poor, due to heat, humidity, pollen, or pollution, staying indoors with windows closed may help prevent symptom flares.
Know Your Triggers
Pay attention to what tends to make breathing harder for you. Common triggers include:
- Extreme temperatures (hot or cold)
- Strong odors, smoke, or fumes
- Physical exertion without rest breaks
- Respiratory infections
- Stress or anxiety
You won’t be able to avoid every trigger, but awareness helps you prepare and respond more effectively.

When Shortness of Breath Is a Sign to Call for Help
Learning to manage symptoms at home is important, but so is recognizing when symptoms need clinical attention.
Consider reaching out to your care team if:
- Breathlessness feels different from your usual baseline
- Your usual strategies (breathing techniques, rest, medication) aren’t helping
- You notice new symptoms alongside breathlessness, such as fever, chest pain, swelling, or changes in mucus color
- You’re using your rescue inhaler more frequently than normal
- Symptoms are interfering with sleep, eating, or basic daily activities
These don’t necessarily mean something serious is happening, but they’re worth a conversation. Early attention to changes can often prevent bigger problems.
If you experience severe shortness of breath, confusion, bluish lips or fingertips, or chest pain, seek emergency care immediately.
How Rotech Healthcare Supports Patients at Home
Managing COPD at home is easier when you have the right equipment, understand how to use it, and know who to call when questions come up.
Rotech Healthcare provides home respiratory equipment, including oxygen therapy, nebulizers, and CPAP/BiPAP devices, along with patient education and ongoing support. Our respiratory specialists help patients understand their therapy, troubleshoot equipment concerns, and stay connected to their care.
Programs like COPDBridge™ offer structured support during transitions from hospital to home, when patients are often most vulnerable to setbacks. And for those managing respiratory conditions long-term, CarePLUS™ provides continued monitoring and care coordination.
The focus is on helping you feel supported, informed, and more confident managing breathing at home.

COPD Shortness of Breath: Common Questions Answered
Why does shortness of breath come and go with COPD?
COPD symptoms can fluctuate based on activity, weather, air quality, sleep, stress, and overall health. A difficult morning doesn’t mean the rest of the day will be hard, and good days don’t mean the condition has improved. Day‑to‑day variability is a normal part of living with COPD.
Is it normal to feel tired after breathing feels difficult?
Breathing with COPD takes more effort than normal, which can lead to fatigue. Feeling worn out after episodes of breathlessness is common. Pacing activities and allowing time to recover can help conserve energy.
What breathing technique helps most with COPD breathlessness?
Pursed‑lip breathing is one of the most effective and widely recommended techniques. It helps slow breathing, keeps airways open longer, and reduces the sensation of air hunger. Practicing it regularly makes it easier to use when symptoms arise.
Should I use oxygen when I feel short of breath?
Only if your healthcare provider has prescribed supplemental oxygen for you. Oxygen therapy is based on specific oxygen levels and needs, and it should not be used “as needed” unless your care team has instructed you to do so.
How do I know when my symptoms are getting worse?
Pay attention to changes from your usual baseline. If breathlessness feels different, your normal strategies aren’t helping, or you notice new symptoms such as fever, increased mucus, or chest tightness, it’s a good idea to contact your care team.
Can anxiety make COPD breathlessness worse?
Yes. Anxiety can lead to faster, shallower breathing, which may intensify the feeling of breathlessness. This can create a cycle where breathing difficulty increases anxiety. Techniques like pursed‑lip breathing can help interrupt that cycle.
What position helps most when I’m short of breath?
Leaning forward, either standing with your hands on a surface or sitting with elbows on your knees, often helps by giving the diaphragm more room to work. The most helpful position can vary, so experimenting is important.
When should I go to the emergency room for shortness of breath?
Seek emergency care if you experience severe breathlessness that doesn’t improve, confusion, chest pain, bluish lips or fingertips, or any symptoms that feel alarming or unfamiliar. If something feels seriously wrong, trust your instincts and get help.
Breathing Easier Starts With Awareness
Living with COPD means adapting to a body that works differently than it used to. That’s frustrating, and some days are harder than others.
But breathlessness doesn’t have to mean helplessness. With practical techniques, thoughtful daily habits, and support from your care team, many people with COPD find ways to manage symptoms and maintain quality of life.
Pay attention to your body. Communicate with the people involved in your care. And know that small, consistent actions often matter more than dramatic interventions.